Alivia Analytics Solutions
SOLVING COMPLEX CHALLENGES
We help health plans and government agencies address financial losses caused by FWA, errors, missed recoveries, fragmented data, and outdated processes.
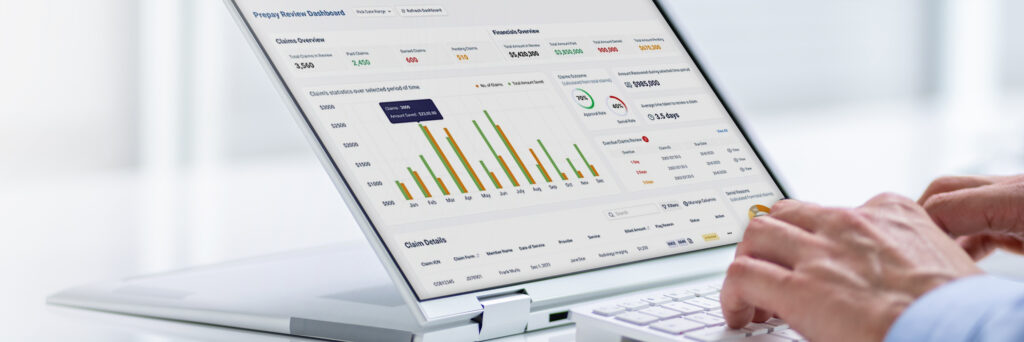
Pre-Pay Preventive Analytics
Our FWA Claims Manager™ flags high-risk providers before payment using advanced scoring, configurable pend-and-review triggers, and built-in compliance checks—helping reduce improper payments and streamline early case review.
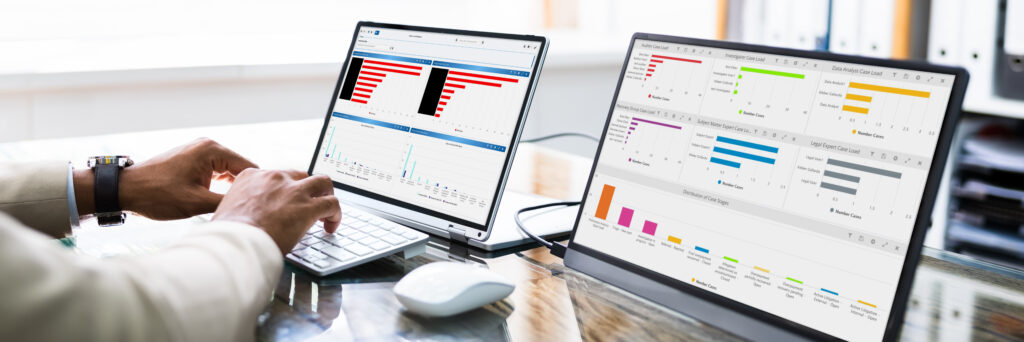
Post-Pay Recovery Analytics
Our FWA Finder™ uncovers hidden leads and accelerates SIU investigations, while Alivia Case Manager™ streamlines case volumes and workflows. Combined with Clinical Audits and Data Mining, we recover more from overlooked FWA and errors.
Innovative Data & IT Services
Our DataChrome™ standardizes claims data into analytics-ready formats and supports all ingestion needs. We also optimize and migrate Claims Systems and Safeguard PHI, advancing payer transformation with secure, scalable infrastructure.