Prevent Improper Payments Before They Happen

Designed for those who demand precision, innovation, and efficiency, our Pre-pay Modules completely reimagine the status quo while powered by Alivia’s latest Generative AI technologies. Scrutinize each claim, revealing a wealth of information in seconds. From billing details to provider information, our configurable model ensures you have the insights to make informed decisions post adjudication, but prior to issuing payment.
- Advanced Data Analysis Post-Adjudication
- Uncover Cost-Saving Opportunities
- Empowered Decision-Making


Comprehensive search interface facilitates quick claim queries, displaying details, billing, and statuses in one view
Pre-Payment Claims Editing
Utilizing Alivia’s platform, our Pre-payment edits integrate with your existing claims adjudication and payment workflows, providing a comprehensive solution for stopping erroneous billing.
Configurable for Tailored Solutions
Our Pre-pay Modules are designed to quickly meet the unique needs of various healthcare payers without compromising data integrity. Robust safeguards ensure that the decision remains untampered, maintaining the sanctity of the audit process.
Transparent & Accountable Decision Tracking
Our platform enriches decision tracking with enhanced visibility, distinguishing between adjudication system decisions and those made within the application, ensuring every stakeholder has a clear view of the process.
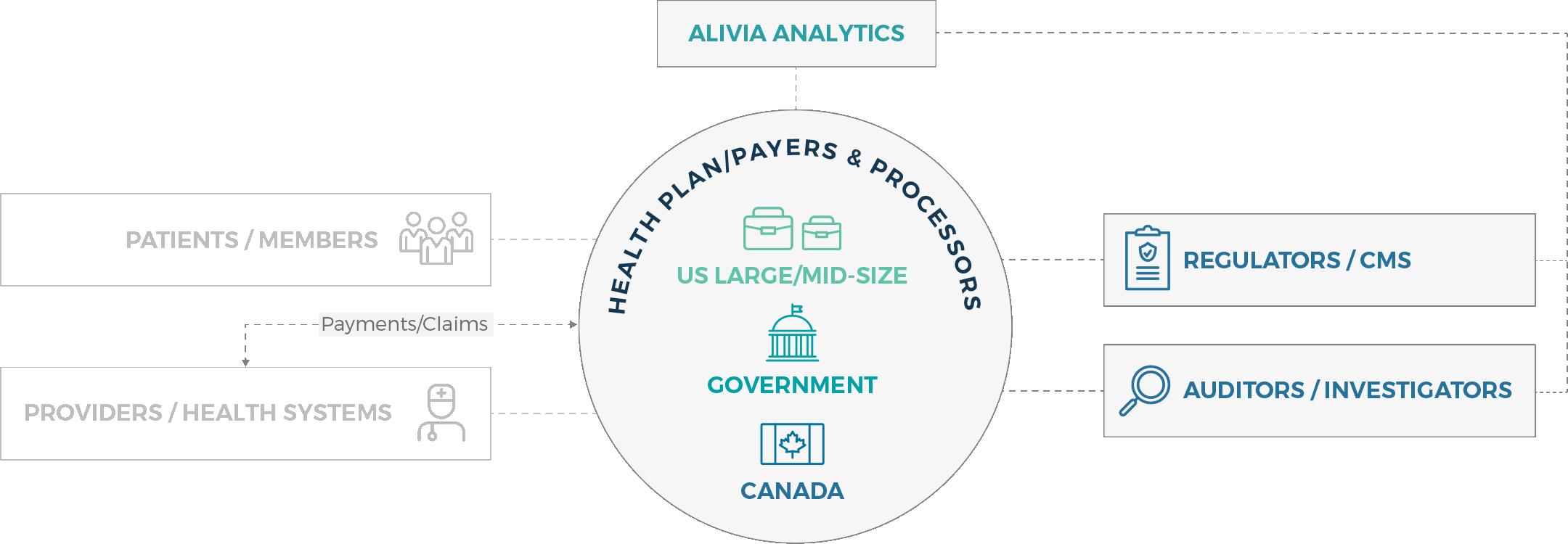
Market focus
Whether you’re a health plan / payer, regulator or investigator, we provide you with seamless analytics solutions that ensure healthcare payment accuracy swiftly and effectively.


Want to see how you can finally achieve healthcare payment integrity?